Recommendations provided here are not intended to replace conversations with your own medical care provider.
Once you have tried simpler, less expensive options to be able to conceive, you may need to look into some more complex infertility treatment options for getting pregnant.
Some people try less invasive infertility treatment options, like IUI (intrauterine insemination), over and over again with no success. Other folks are unable to try and conceive without more invasive intervention for a number of reasons. For both of these groups of people, sometimes the best option for growing their family might be in vitro fertilization.
In vitro fertilization, or IVF, is the process of introducing eggs and sperm to each other in a lab instead of in their natural environment.

The process begins with a medication protocol designed to stimulate multiple follicles on each ovary to grow, instead of just the one or two that develop with less medical intervention in an ovulation induction or IUI cycle. There are a few different ways to do this. Your provider will determine the best protocol to use based on your history and test results.
The ovaries are stimulated to grow multiple follicles by using injectable medications called gonadotropins.
These medications are synthetic forms of hormones that are produced by the body to grow an ovarian follicle to maturity when it will release an egg. By giving a higher dose of these hormones, the ovaries are stimulated to grow more follicles, each of which contains and releases an egg.

Women who are undergoing stimulation for IVF require close monitoring to make sure that they are taking the right dose of medication, and to make sure that they don’t ovulate before their eggs can be harvested for insemination in a lab.
The monitoring consists of ultrasound to count and measure the ovarian follicles, and blood work to measure hormone levels. Based on those results, the provider can determine if a woman needs to change her dose of stimulation, or if she is ready to prepare for her egg retrieval.
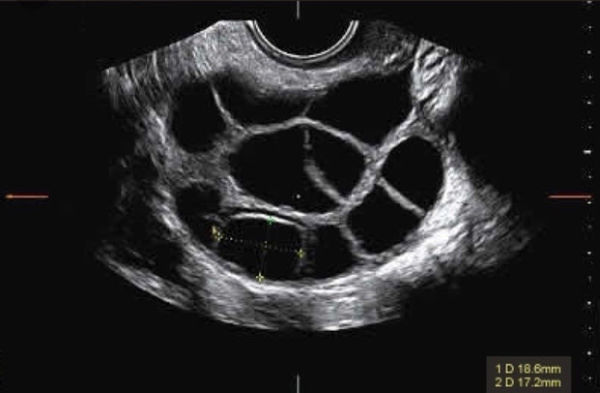
When the ovarian follicles have reached maturity, the provider will determine the best time for the final set of “trigger” injections. These medications cause ovulation to begin and give the eggs a final boost of maturation before they are removed from the follicles. This “trigger” is timed very precisely so that at the retrieval, the eggs are ready to be removed.
Egg retrieval is a minor surgical procedure done under anesthesia.
An ultrasound is used to guide a hollow needle into the follicles. The fluid in the follicles is drained and taken to the lab. The embryologist will look at the fluid under the microscope and count the number of eggs that have been removed from the follicles. This procedure usually lasts about 30 minutes. Most women have some mild discomfort after their egg retrieval.

Once in the lab, the eggs will be inseminated by sperm, either collected from the male partner or thawed from a donor sample.
The next day, the embryologists will see how many of the eggs have fertilized to become embryos. Over the course of the next few days, the development of the embryos will be monitored in the lab to see how they develop.

The embryo transfer will take place 2-5 days after the retrieval.
The timing of the transfer and the number of embryos to be transferred depends on the number and quality of the embryos created. Using an abdominal ultrasound, the provider will guide a thin catheter containing the embryo (or embryos) into the thickest part of the uterine lining. The transfer usually takes less than ten minutes, and there is no anesthesia or sedation required. The pregnancy test will be scheduled about 10-13 days later. Any remaining embryos that meet the facility’s specific criteria on day 5 or 6 of embryo development will be frozen and stored for potential future use.
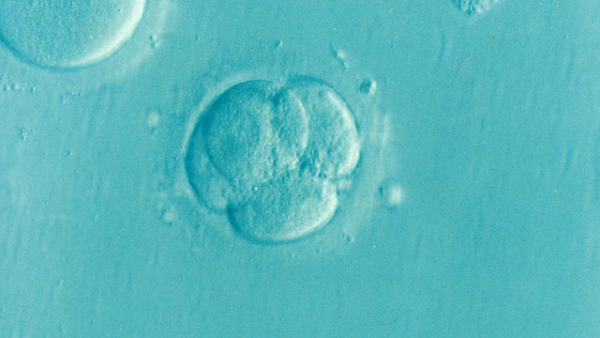
It’s important to consider the emotional aspects of this kind of infertility treatment. Patients can experience a spectrum of different feelings while considering IVF as a treatment option, as well as once they embark on the cycle.
Excitement and anticipation about undergoing a treatment that may give a higher chance of success can be tempered by fear of more failure, apprehension over the injections and procedures, and a further loss of control over what others achieve naturally. All of these emotions are perfectly normal, and it’s okay to reach out for support from loved ones or professionals.
Every facility, and every provider, has their own specific criteria and protocols to maximize the best outcome for each patient who is considering IVF. It’s important to be aware of what to expect with your specific treatment plan and to ask questions along the way so that you are an active member of your infertility treatment team.
Vermont Mom would like to thank Vermont Surrogacy Network for making this series possible.
Pin this post and be sure to follow Vermont Mom on Pinterest!